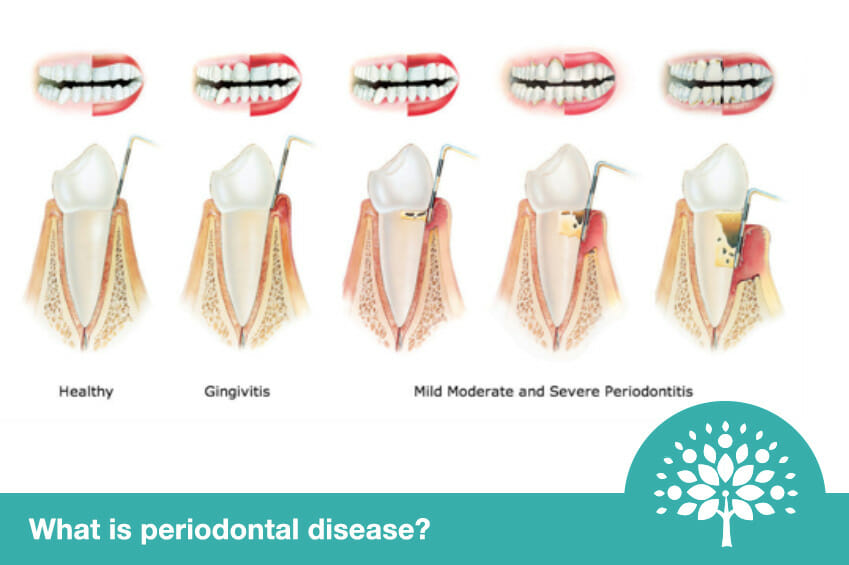
What is periodontal disease?
Periodontal disease is an inflammatory disease. The inflammation is part of the body’s natural defence mechanisms and occurs in response to a build-up of plaque (bacteria) on the teeth. In some patients, this natural inflammatory process is too severe or poorly controlled and the inflammation actually damages the supporting structures of the teeth, namely the gums and supporting bone. Whilst we can control this process and stop the bone loss from getting worse, the bone loss is usually irreversible.
Who gets periodontal disease?
Approximately 10% of the population are severely affected by periodontal disease and by the age of 60 years old around 80% of people will display some bone loss, albeit mild. There appears to be some genetic link with periodontal disease, with trends running in families. If you have been diagnosed with periodontal disease, then potentially your siblings are at increased risk of having the same problem and potentially your children may also be at increased risk. Ideally, they should all be screened and monitored for potential problems by their dentist.
Does anything make it worse?
The single biggest risk factor for developing gum disease, after poor oral hygiene, is smoking. Smokers lose three times more teeth than non-smokers and they do not respond as well to treatment as non-smokers. There are other conditions such as poorly controlled diabetes, poor diet or stress that can also play their part. Stopping smoking is a very important part of controlling this disease and preventing tooth loss. Should you wish to quit smoking, the best people to speak to would be your GP or local stop smoking clinic. We are also happy to offer advice.
Can it be treated?
Periodontal disease can be treated successfully; however, we cannot cure it. Similar to diabetes, there is no cure, but by stabilising the disease, we can prevent further damage and allow you to keep your teeth for a long time.
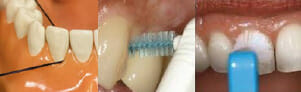
What can I do to help?
Your role in the management and stabilisation of the disease is crucial. We will show you techniques aimed at helping you clean your teeth to a very high standard so that the bacteria levels are below the level that triggers inflammation. This is different from one patient to the next. Without this change in home care, our treatment cannot be successful. Controlling the risk factors outlined above is an important part of helping yourself control your disease.
What if I don’t have treatment?
If the bone loss around the teeth is not controlled, then teeth may become loose, gums may shrink and, in some cases, teeth may become infected or even fall out.
What does treatment involve?
Once you are successfully controlling the plaque build-up, we will help by removing the deposits that you cannot reach or are firmly attached to the teeth. This can take time and you may require several treatment sessions over a period of many months depending on how severe the disease is. It is impossible to know how long it will take to stabilise the condition but the harder you work at home the quicker things tend to happen.
If it is about bacteria, why can you not just give me antibiotics?
This is not an infection, it is the body’s reaction to removable plaque. When the plaque is physically removed by you and by us, the inflammation will resolve and the disease will stabilise without the need for antibiotics. Gum disease is almost never treated with antibiotics.
Are there any side effects to treatment?
Due to the fact that there has been irreversible bone loss, when the inflammation resolves it is likely that you will experience some gum shrinkage and possibly some sensitivity. These are unavoidable side effects of treatment, but you must remember that failing to control the disease may result in tooth loss.
If you think you have periodontal disease then please book an appointment at Oakley Road Dental Practice.